
Wisdom teeth removal and extraction surgery
Wisdom teeth, also known as the third molars, are the last molars on each side of the jaws. As they are the last permanent teeth to emerge or erupt, usually when a person is between 18 and 25, there is often not enough room left in your mouth to accommodate them. In fact, they can become a problem if they cause crowding in your mouth, erupt in the wrong position, or become impacted. Not everyone keeps these teeth, nor are they necessary for having a healthy, beautiful smile.
Problems with Impacted Wisdom Teeth
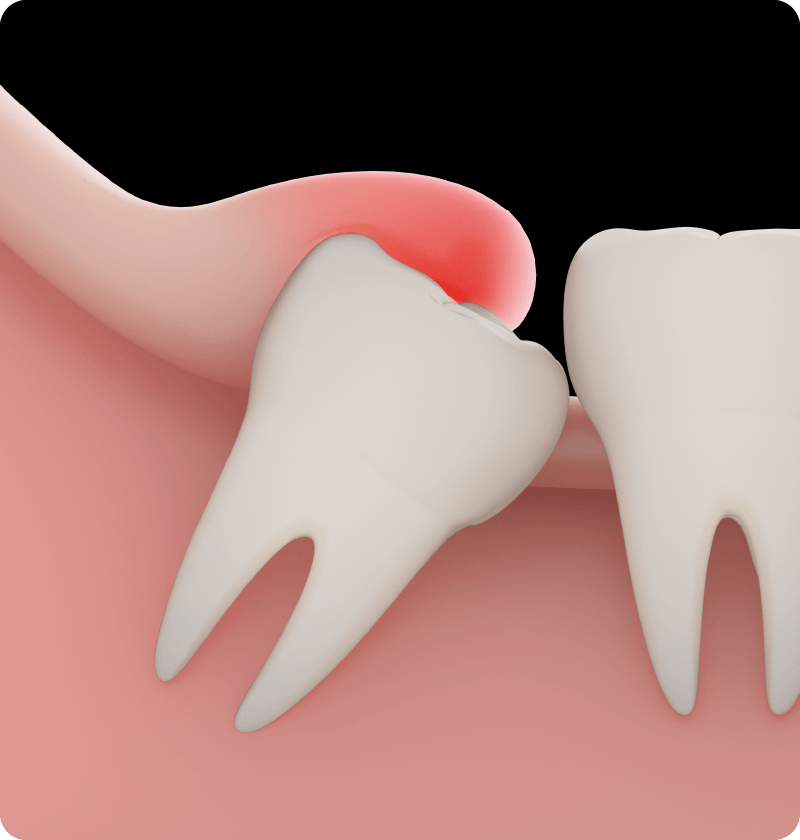
Pericoronitis
Pericoronitis is inflammation of the tissue surrounding a wisdom tooth. The common condition most often occurs in lower molars that are partially impacted, or not fully visible. Periodontal tissues easily get inflamed due to the build-up of food debris and bacteria between the crown of the wisdom tooth and the gums that cover it, as well as the location of the tooth, which prevents the patient from cleaning it thoroughly. Inflamed gums are often damaged by biting. The symptoms of pericoronitis include severe pain, discharge of pus, bad breath, swollen lymph nodes under the jaw, lockjaw and pain when swallowing.
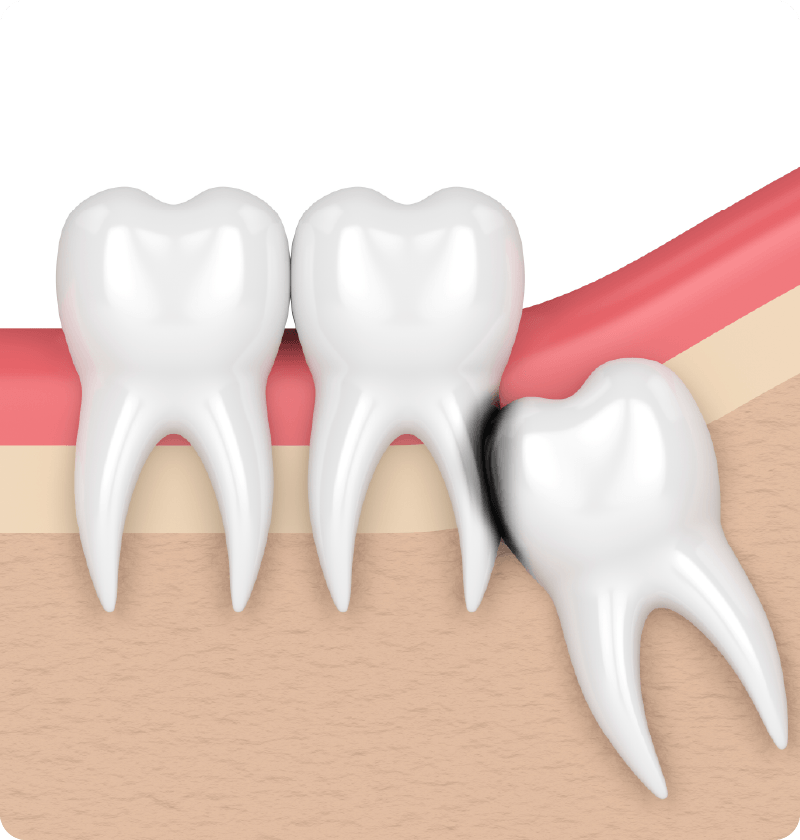
Tooth Decay
Difficulty in cleaning the area between the impacted wisdom tooth and the adjacent tooth. A build-up of plaque can lead to the decay of both teeth.
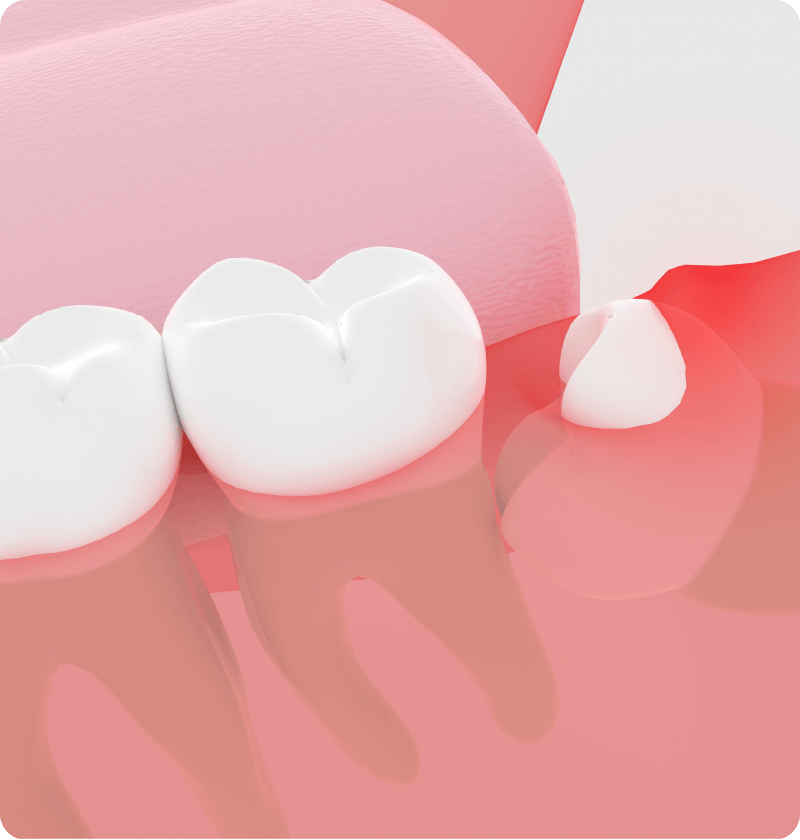
Root Resorption of the Adjacent Tooth
Inflammation of periodontal tissues and impacted wisdom teeth can put pressure on the adjacent teeth, causing the roots of the adjacent teeth to shrink.
Wisdom tooth surgery can be classified as preventive or curative. Generally speaking, wisdom teeth that have not come in properly can trap food debris easily and make it difficult to clean. This gives cavity-causing bacteria a place to grow and for infection. For the above reasons, some may decide to remove the wisdom tooth to prevent its dental problems. For patients with decayed, abscessed wisdom teeth, inflamed gums or cysts, as well as resorption of the adjacent tooth sockets, they need to have their teeth extracted.
What to Expect - Before and During the Procedure
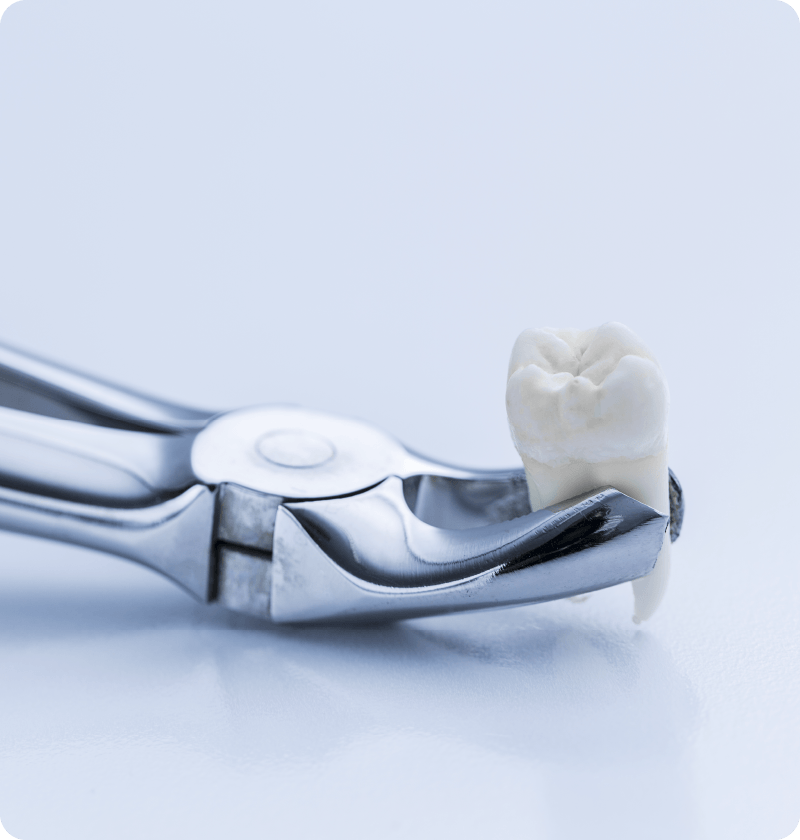
In some cases, the roots of wisdom teeth are deeply embedded in the jawbone and close to the main nerves. Extraction can damage the nerves, resulting in numbness and loss of sensation in the mouth. The dentist will balance the risks of extraction against the clinical situation, diagnosis and the patient's decision before the surgery.
The procedure is usually carried out under local anaesthetic and sometimes under general anaesthetic or sedation. Normally, you won’t feel any pain during the surgery. Once the patient is under anaesthesia, the dentist will make an incision in the gum tissue to expose the tooth and bone, remove bone that blocks access to the tooth root, divide the tooth into sections if it's easier to remove in pieces and remove the tooth.
Points to note
It is common to experience discomfort after surgery. Follow your doctor's instructions on recovery.
On the day of surgery
Avoid touching the wound, gargling and brushing the teeth. Eat soft foods for a few days and chew with the jaw on the other side. Avoid doing strenuous activity. Do not smoke or drink alcoholic beverages. On the next day, patients can brush their teeth and chew on both sides as usual.
After surgery
Wound pain, facial swelling and difficulty opening the mouth are common symptoms. Apply an ice pack against your cheek to help relieve pains and apply a warm towel to the swollen area to reduce discomfort on the second day. Maintain oral hygiene to prevent wound infection. Eat soft foods for three days or four following the surgery. Take painkillers as prescribed by the dentist if you experience pain after surgery.



 Clinic Location
Clinic Location



